Shingles, a frequently misunderstood condition, represents a stealthy “assassin” that lurks in our midst, poised to strike not only the elderly but anyone susceptible. The varicella-zoster virus (VZV), upon initial infection, manifests as chickenpox before lying dormant within the body, potentially reactivating later to unleash the painful rash of shingles.

Who bears the brunt of this disease?
1. The Elderly: Immune systems naturally weaken with age, making individuals over 50 more vulnerable to shingles.
2. Immunocompromised Individuals: Those with HIV, cancer patients undergoing chemotherapy or radiotherapy, and organ transplant recipients on immunosuppressants face heightened risks.
3. Prior Chickenpox Sufferers: Anyone who has had chickenpox is at risk due to VZV’s latency in the nervous system, which could reactivate at a later time.
4. Long-term Corticosteroid Users: People with autoimmune disorders like rheumatoid arthritis or lupus may be more susceptible.
5. Stressed Individuals: Prolonged stress, whether mental or physical, can weaken immunity and increase the likelihood of developing shingles.
6. Transplant Recipients: Patients who have undergone organ or bone marrow transplants and require immunosuppressive drugs to prevent rejection are particularly at risk.
This list is not exhaustive, and other factors may influence an individual’s susceptibility to shingles.
The Incubation Period of Shingles
The incubation period of shingles spans from the initial VZV infection to the onset of symptoms, varying from weeks to years, depending on factors such as immunity and viral load. During this period, the virus replicates silently without causing noticeable symptoms until it reactivates when the immune system weakens. Thus, even if you’ve been symptom-free for decades, the possibility of harboring the virus cannot be ruled out.
The Course of Shingles
1. Initial Infection: An individual typically contracts chickenpox upon initial VZV infection.
2. Viral Latency: Post-chickenpox, VZV doesn’t leave the body but lies dormant in the nerve ganglia of the nervous system.
3. Reactivation: Years later, due to waning immunity or other triggers, these latent viruses may become active again, traveling along nerve paths to the skin’s surface and causing shingles.
Characteristics of Shingles Reactivation include:
1. Prodromal Symptoms: A few days before the rash appears, people may experience pain, itching, or tingling sensations, usually localized to a specific area of skin.
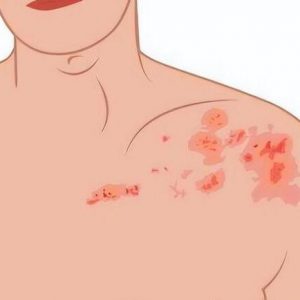
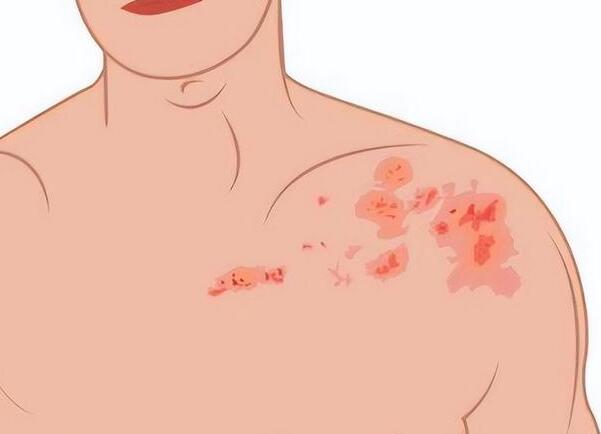
2. Rash and Blisters: Subsequently, the affected area develops redness, progressing to painful blisters that eventually crust over and heal.
3. Symptom Duration: While the rash typically heals within 2 to 4 weeks, the pain may persist beyond the blisters’ resolution, a condition known as postherpetic neuralgia (PHN).
Should symptoms resembling shingles arise, prompt medical consultation for diagnosis and treatment is essential.
Preventing Shingles
1. Vaccination: The most effective prevention is vaccination against shingles. Several vaccines are available, including the recombinant Shingrix and the live Zostavax vaccine. The recombinant vaccine is generally superior, offering better protection and recommended for adults over 50.
2. Immunity Boosting: Maintaining overall health can also deter shingles since recurrence correlates with weakened immune function.
Balanced diet, regular exercise, adequate sleep, stress reduction, and avoiding smoking and excessive drinking can help fortify immunity.
3. Early Intervention: For those experiencing prodromal symptoms, timely medical attention can mitigate severity. Antiviral medications like acyclovir, valacyclovir, or famciclovir can slow viral replication in the early stages.
4. Education and Awareness: Knowing about shingles and its complications, such as PHN, enables rapid action upon symptom detection.
5. Managing Chronic Diseases: Properly managing chronic conditions like diabetes or heart disease can reduce the risk of shingles as these diseases impact immune function.
Individual circumstances vary, so consulting healthcare professionals is crucial to determine the most suitable prevention strategy.
Treating Shingles
1. Antiviral Medications: The first line of defense against shingles, these drugs reduce viral replication and may shorten the disease’s course and alleviate symptoms, including acyclovir, valacyclovir, and famciclovir. These are most effective when administered within 72 hours of the rash’s onset.
2. Pain Management: Shingles can cause significant pain, potentially managed with:
Over-the-counter pain relievers like ibuprofen or acetaminophen
Prescription painkillers such as codeine
Topical agents like lidocaine patches
Tricyclic antidepressants (for persistent pain control) like amitriptyline
3. Skin Care: Keeping the skin clean and dry helps prevent infections and avoids irritants. Cool wet compresses or baths may offer relief.
4. Neurological Medications: In severe cases, doctors might prescribe antiepileptic drugs like gabapentin or pregabalin to address neuropathic pain associated with shingles.
5. Immunological Support: Immunocompromised patients may require additional support, such as immunoglobulin therapy.
Before using any medication or treatment strategy, always seek advice from a physician or healthcare professional to ensure the plan suits your situation and monitor its effectiveness. Moreover, even during treatment, avoid contact with those who have never had chickenpox or have weakened immune systems to prevent VZV transmission.
As a complex and potentially painful disorder, shingles demands vigilance. By recognizing high-risk groups and signs of the incubation period, we can prepare accordingly, striving to sidestep this invisible health landmine.